So, if you’ve read any of our previous blogs you’ve probably identified a common theme amongst our topics. The Ozark Regional Vein & Artery Center often tries to answer patient questions that we’ve heard a bunch. This month, we’re taking a slightly different approach—we’re pre-empting your questions.
Many patients who come to us were referred by their primary care provider or loved one, and already know they have vascular issues they need help with. Well, plenty of folks aren’t sure what they’re dealing with or if their health concerns are vascular in nature. That’s why we wanted to take time to highlight the venous insufficiency symptoms everyone should be on the lookout for.
This blog will outline the root of many vascular conditions, venous insufficiency, and detail the 6 major symptoms you should be looking for.
Venous Insufficiency. What is it?
Venous insufficiency, also known as venous reflux disease, is a form of venous disease that occurs when veins in your legs are damaged. As a result, these veins can’t manage blood flow as well as they should, and it’s harder for blood in your legs to return to your heart. Venous insufficiency causes blood to pool in your leg veins, leading to high pressure in those veins.
Venous Insufficiency can happen due to damage in any of your leg veins, including your:
- Deep veins: which are large veins deep in your body that run through your muscle.
- Superficial veins: which are close to your skin’s surface.
- Perforating veins: which connect your deep and superficial veins.
Venous insufficiency may cause mild symptoms at first. But over time, this condition may interfere with your quality of life and lead to serious complications.
So, what are the venous insufficiency symptoms you need to be on the lookout for? We’re happy to tell you!
Venous insufficiency symptoms
1. Cramping
One of the first symptoms of venous disease is leg cramping. It’s your veins’ job to transport blood back to your heart once your heart pumps it throughout your body. When your veins start failing in this task, also known as venous insufficiency, it can lead to a variety of symptoms. Leg cramping is one of the first and the most common.
At night when you’re laying in bed for an extended period, the slowing or stagnant blood flow as a result of venous insufficiency can result in increased discomfort and site-specific pain. The exact reason for this isn’t apparent, but there is a direct correlation between the onset of night-time leg cramps and venous disease.
That said, cramping has numerous causes. Muscle overexertion, dehydration, strain, or holding a position too long—all these causes are just as likely the reason for your leg cramps.
If you’ve been on your feet all day and when you plop down for bed, you notice leg pain, it’s not reasonable to assume the presence of venous insufficiency. It’s essential to think critically about your body’s health. So, if you’re noticing that you’re frequently feeling leg cramps at night as you try to go to sleep, no matter what you’ve been doing, that’s something to mention to your healthcare provider or a vascular specialist.
For more information, consider using our virtual screening questionnaire to take an active role in your vein health!
2. Restless Legs
Venous insufficiency symptoms are consistent in their impact on the lower extremities. Restless Leg Syndrome (RLS), is no exception, and often acts as an extension of symptomatic leg cramping. Characterized by the uncontrollable urge to shake or move your legs, RLS often manifests in the evenings and can lead to incredible difficulty falling asleep or staying asleep. RLS sufferers also report feeling tingling, itching, and pins-and-needles sensations in their legs.
Though various issues can cause RLS, not purely problems with your veins, venous insufficiency can lead to restless legs as the faltering blood valves cause blood to pool in the legs and create discomfort.
Just as with leg cramps, it’s important not to overanalyze and start seeing issues where none exist. The occasional urge to bounce or shake your leg to distract yourself or vent extra energy is normal. If the urge is significantly interfering in your life, though, you should consult your healthcare provider.
3. Painful Varicose Veins
Varicose veins are one of the most common signs of broader venous insufficiency. Blood that’s not being pumped back to the heart begins to pool or reflux in the veins of your legs and ankles, leading to discolored, bulging varicose veins that protrude against the skin.
The CEAP (Classification, Etiology, Anatomy, and Pathophysiology) is an official standard of classification, followed by vein experts across the country, to classify the severity of your vein issues on a scale of 0-6. C0-C1 are cosmetic issues with virtually no meaningful health effects, and stages C2 and higher are more serious health concerns of increasing severity.
Even though the development of varicose veins is stage C2 of the CEAP scale, there is a common misconception that varicose veins are benign and purely a cosmetic concern. While varicose veins are a natural part of growing older and not always an immediate problem, they can cause leg pain and achiness and become an ongoing health issue if left untreated.
Check out other misconceptions about varicose veins→
Though their removal isn’t always necessary, varicose veins may start forming as early as your 20s and indicate other serious issues. Thankfully, if you’re dealing with uncomfortable or painful varicose veins, you have a large selection of treatments for varicose veins and venous reflux with the vascular specialist in Rogers at the Ozark Regional Vein & Artery Center.
4. Spider Veins
This is one of the most common venous insufficiency symptoms. What complicates matters, however, is that spider veins are also common in older patients without serious venous concerns.
Spider veins can be blue, purple, or red. They may appear in the form of thin lines, webs, or branches. People sometimes also refer to them as thread veins. Typically, they are not painful or harmful, but some people may wish to treat them for cosmetic reasons.
While not a problem in and of themselves, spider veins are very frequently a sign of other vascular concerns lurking behind the scenes. So, while there’s no need to panic if you see any crop up, it’s worth consulting your medical provider or receiving screening.
If you’re looking for vascular screening, feel free to contact us to schedule a consultation. Or you can take advantage of our virtual screening questionnaire to jumpstart the treatment process!
5. Swelling
Are your legs swollen and even painful? Swelling can be an indicator of vein disease progressing in your body. Venous insufficiency can become deadly if left to progress without intervention. If you are experiencing swollen legs, learning about vein disease could save your life and improve the quality of the life you live.
If you are experiencing chronic swelling in the legs, ankles, or feet, vein disease might be to blame. Venous edema is the term for this swelling when vein issues cause it. Over 90% of swollen legs are due to vein health, so chances are, if you have been experiencing this, the cause is venous insufficiency.
Swelling occurs because blood flow through the vessels is impaired. Fluid is then able to accumulate with no release, and this often happens in the legs.
Signs of edema in the lower limbs:
- Cyclical swelling of one or both limbs
- Is sometimes painful
- Swelling and/or pain worsens with prolonged standing
- Symptoms improve with raised legs
- Over time, the skin may thicken in the area
- The limb may begin to feel hot when standing
- Legs may feel heavy, and this feeling can increase when standing or moving
When edema is from vascular disease, you will often find spider veins, darkened skin, eczema, and ulcers in the surrounding area. Lymphedema may also develop when the lymphatic system can’t drain properly.
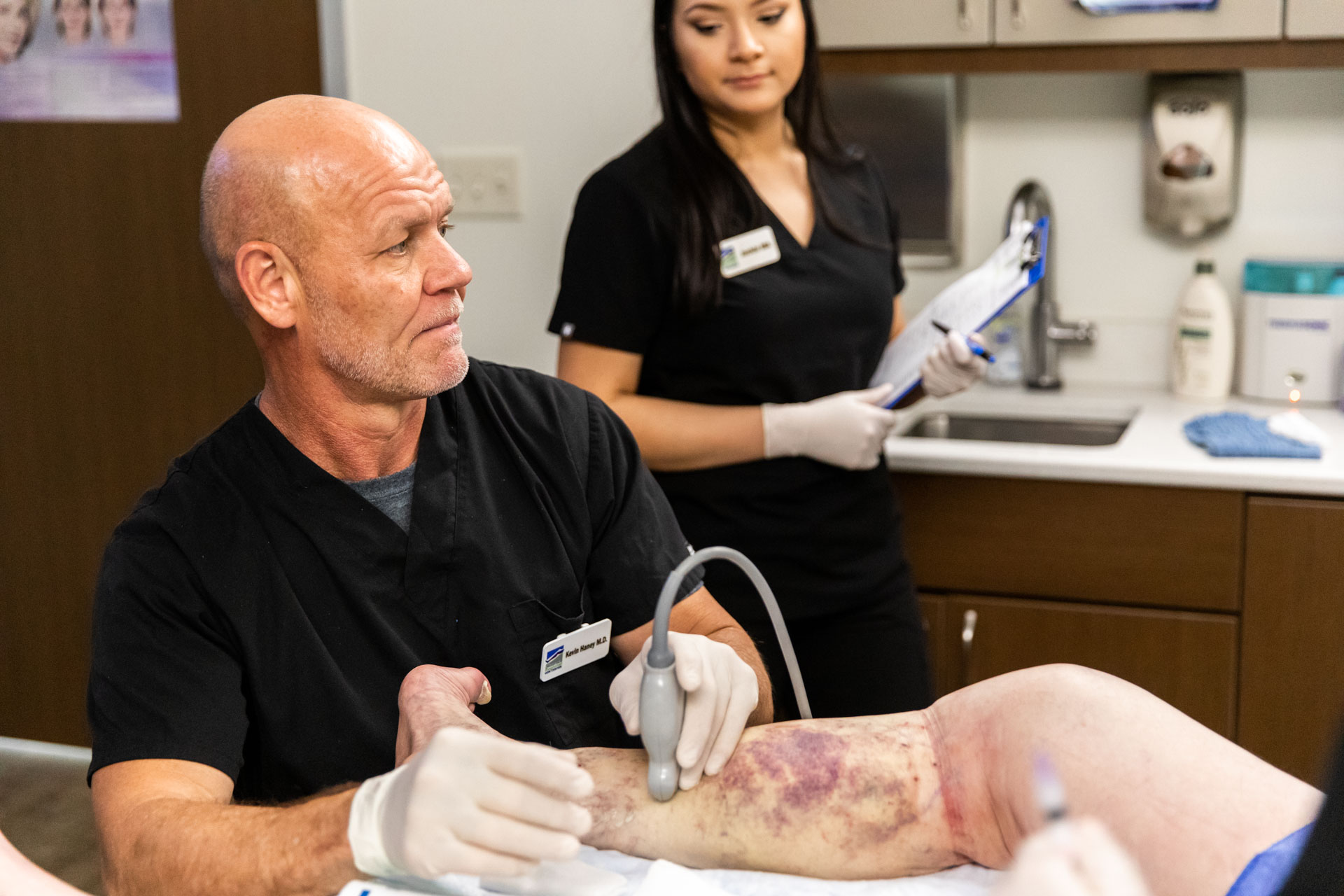
6. Discoloration
You may notice that the skin on your lower legs becomes discolored or appears bruised as you age. The technical term for this is hemosiderin staining. It’s often caused by chronic venous insufficiency. You may need to make lifestyle changes to help fix the condition.
Hemosiderin staining looks like a patch of skin that is a darker color than the surrounding skin. It can look like bruising, or it can be brownish or rust-colored. It may be harder to spot if you have a dark skin tone. Over time, the discoloration may become darker and look nearly black.
Discoloration usually happens on the lower leg, near the ankles, or on your feet. It’s caused by blood leaking out of the tiny vessels called capillaries. The blood pools under the skin and leaves a residue of hemoglobin that settles in the tissue there. Hemoglobin contains iron, which causes the rusty color of the stains.
Get Support To Tackle Your Venous Insufficiency Symptoms
If you require support tackling your venous insufficiency symptoms, come to the Ozark Regional Vein & Artery Center. Our experience and growing suite of care options enable us to guide you toward lasting wellness solutions for a happier, healthier life.
We are the premier practice in Northwest Arkansas for all the highest-quality vein treatments available. Patients come to Dr. Haney, Dr. Stout, and the expert staff from all over Northwestern Arkansas, from Fayetteville to Bentonville, to ensure they receive the best concierge-level care and leg vein procedures.
Lead the charge on your vascular care with our Virtual Vein Screening Tool or by scheduling a consultation.