Your body is home to a complicated superhighway of veins and arteries. They transfer blood all around the body, and they’re a vital part of our bodily function.
And although the vein system is a necessary part of our biology, most of us don’t know much about how it works. We don’t think we need to! And you probably don’t need to—that is, until you need treatment for a vein and artery disorder.
At Ozark Regional Vein & Artery Center, we can help you treat vein disorders like pelvic venous congestion syndrome. We have years of experience in this field, and we want to help you receive the treatment you deserve.
The Vein System
You have a lot of veins. Probably more than you’d think. If you were to take every single one of your blood vessels and stretch them end to end, they could circle the globe twice! They’re always busy, too.
Every single day, your heart pumps 1,800 gallons of blood through your vessels. With that much hardware, it shouldn’t be a surprise that things can go wrong. Blood vessels are a complicated part of the body, but our bodies aren’t perfect. They can’t predict and prevent every single problem. So that’s where our team can help.
Meet the Ozark Team
The team at Ozark is top of the line. We understand that most people don’t know how to take care of their veins and arteries as effectively as they should, so we’re there to help when things don’t go according to plan. We have lots of different treatment options available for several different vein and artery disorders, including pelvic venous congestion syndrome.

With our capable crew by your side, you won’t have to go it alone. When you meet with us, we treat you like a valued member of our team, because you are! We’re nothing without our incredible patients, so we’ll do our best to make your experience at Ozark rewarding.
Disorders and Treatments
Before we discuss pelvic venous congestion syndrome, we’ll go over some of the other most common vein & artery disorders we see at Ozark. We’ll also discuss how we can treat these disorders.
Consultation
Before we commit to any treatment strategy, we have to complete a brief but in-depth consultation. We don’t want to waste your time and schedule a treatment that isn’t absolutely necessary for solving your vein and artery disorder.
We’ll ask you some questions and complete a physical exam that will give us more information about symptoms. Once we determine what you’re dealing with, we can begin formulating a treatment plan designed to help you feel better.
May-Thurner Syndrome
One of the disorders we treat is May-Thurner syndrome. May-Thurner syndrome occurs when your right iliac vein puts pressure on your left iliac vein. These veins pump blood to and from the heart, respectively.
When pressure is put on these veins, the normal processes stop, and blood flow is interrupted. This may cause the blood to actually pool inside your legs, which increases the risk of blood clots and deep vein thrombosis. Deep vein thrombosis (DVT) can result in a pulmonary embolism, which can be fatal.
May-Thurner syndrome is a common disorder; it actually occurs in about 20% of all people. May-Thurner can result in several irritating side effects, including:
- Bulging leg veins
- DIscolored leg skin
- Leg pain
- Leg swelling
None of these specific side effects are life-threatening, but they could be indicators that you are suffering from the aforementioned DVT, which is a serious and potentially deadly condition. If you notice these symptoms, it would be a good idea to schedule a consultation with our vein & artery center. From there, we can get started on your treatment.
Angioplasty
We can treat May-Thurner syndrome through angioplasty. Angioplasty is a complicated—but intuitive—procedure designed to clear blockages in the veins. First, a catheter is inserted into the artery.
This catheter actually has a small balloon attached to the tip. When this catheter reaches the blockage, our angioplasty expert, Dr. Christopher Stout, expands the balloon. This opens up the artery, giving Dr. Stout the ability to clear the blockage.
We may also decide that a stent is necessary to keep the artery open while we work. Angioplasty can be a very effective solution for May-Thurner syndrome.
Uterine Fibroids
Aside from pelvic venous congestion syndrome, we also offer treatment for uterine fibroids. Uterine fibroids are growths that form in your uterine tissue. These growths aren’t cancerous, and they’re prevalent in many women.
Unfortunately, we aren’t yet sure what causes uterine fibroids, though hormones like estrogen may contribute to their growth.
Uterine fibroids look different from person to person. They can range from half an inch to six inches in diameter. The largest uterine fibroids may actually fill the pelvis entirely. Certain medications, like birth control, may result in this growth. Uterine fibroids may actually shrink as women get older and enter menopause.
Uterine fibroids can result in several symptoms, including but not limited to:
- Pain in the abdomen
- Heavier periods
- Longer periods
- Cramps
- Excessive urination
- Pain during sex
- Swollen uterus
- Constipation
As you can see, the symptoms stemming from uterine fibroids are extremely varied. If you think you may be suffering from some of the more adverse symptoms of uterine fibroids, you can get diagnosed through a routine pelvic exam.
Uterine Fibroid Embolization
Uterine fibroid embolization is a minimally invasive procedure designed to lessen the intensity of uterine fibroid symptoms. First, a catheter is inserted into an artery or vein and then snaked to the predetermined treatment location.
From there, Dr. Stout will block the blood vessels leading to the uterine fibroid. Then the fibroid is cut off and slowly reduces over time. After six months, you might see a 50% reduction in your fibroids, and by the end of the treatment plan, you can see a 90% reduction!
Pelvic Venous Congestion Syndrome
Another one of the disorders we treat is pelvic venous congestion syndrome. As the name suggests, this disorder stems from problems with your pelvic veins. The pain occurs when your pelvic veins become twisted, tangled, and swollen with blood.
One of the major symptoms of this order is chronic, long-lasting pain in the pelvic area. Like May-Thurner syndrome, pelvic venous congestion syndrome is very common. Your risk for this disorder increases if you have varicose veins, if your family has varicose veins, or if you’ve given birth more than once.
The majority of women who have this disorder are 20 to 45 years of age, but if you’re experiencing menopause, your likelihood of getting this disorder decreases drastically.
The pain associated with pelvic venous congestion syndrome can vary. Some describe the pain as sharp, but most say it feels achy and dull. The pain may also be centralized on your left side, right side, or both, but most commonly, the pain is situated entirely on the left.
Aside from chronic pain, you may notice:
- Accidental urination, or stress incontinence
- Diarrhea or constipation
- Pain when urinating
- Varicose veins
These symptoms are not exclusive to pelvic venous congestion syndrome, so if you’re suffering from any of the above ailments, consider reaching out to a medical professional.
Sclerotherapy
One of the ways we can treat pelvic venous congestion syndrome is through sclerotherapy. Sclerotherapy takes a simple approach to treating swollen, engorged veins. It just collapses them altogether.

Don’t worry if the idea of collapsing a vein sounds a little dangerous. The body has methods of redirecting blood flow and absorbing the collapsed vein. It’ll be like it wasn’t even there in the first place.
Sclerotherapy is a minimally invasive treatment that can be done quickly, and you won’t need to wait around for long post-treatment operations. We want you to get back to your life as soon as possible.
The Injections
The major part of any sclerotherapy procedure is the injections. When administered correctly, the sclerotherapy injections will collapse the swollen veins, causing them to break down.
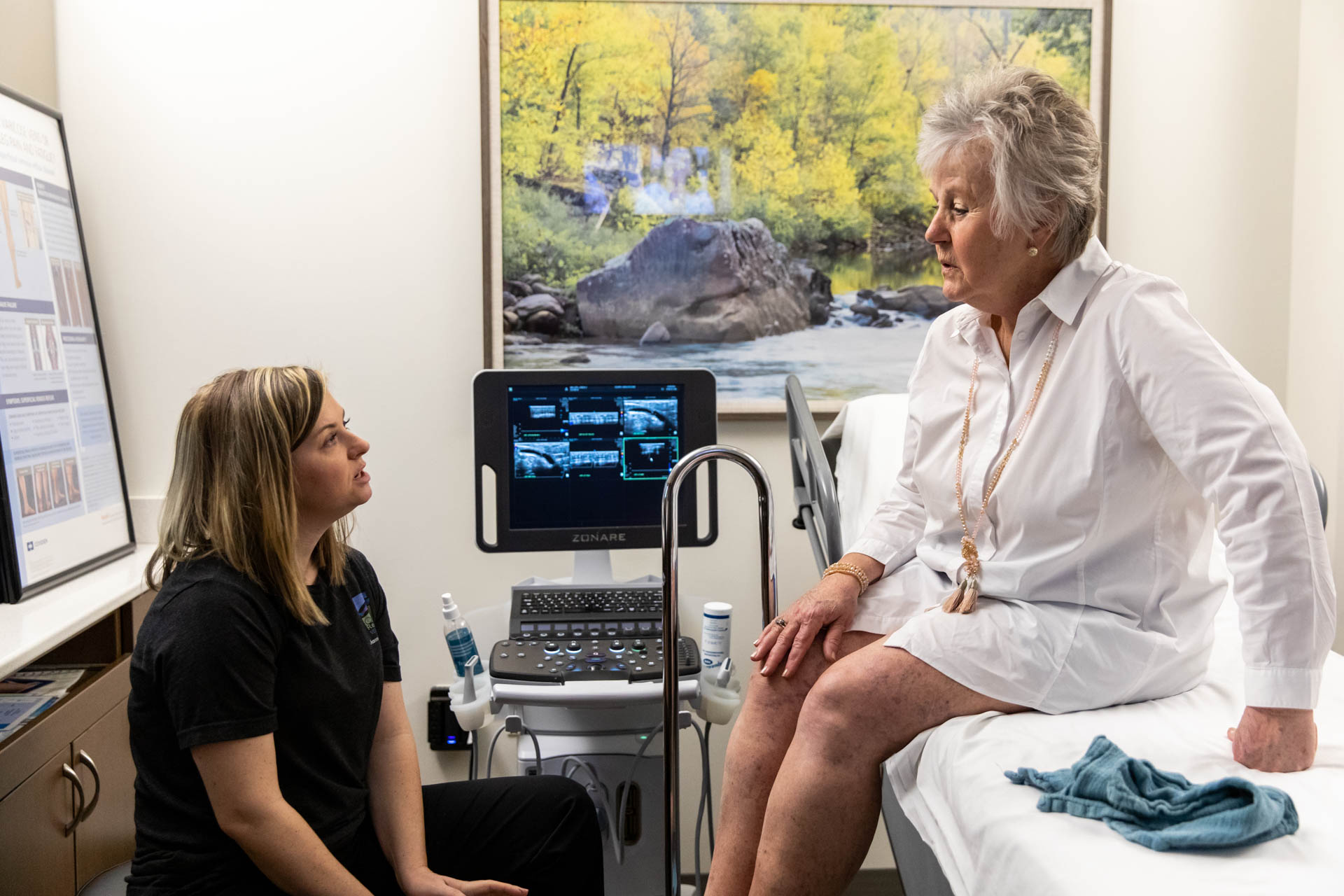
To ensure that he’s injecting the veins in the correct areas, our sclerotherapy expert, Dr. Haney, might utilize an ultrasound, just like the ones you’d use at a pregnancy check-up. This ultrasound allows Dr. Haney to see below the surface of the skin, so he can be as accurate as possible during your procedure. We want to minimize any potential risks whenever we can.
The Aftermath
After your sclerotherapy procedure is complete, some of your more visible symptoms, like varicose veins, might still show on the surface of the skin. Don’t be concerned—this isn’t a sign that your treatment is ineffective. It just may take a while before your symptoms disappear.
Your varicose veins may still show for weeks after the procedure. Just be patient. You’ll also want to take some minor precautions following the treatment to ensure your body heals effectively. Don’t take any long flights, and try to avoid any particularly warm temperatures, like those you might find in a sauna or hot tub.
Reach Out to Us About Vein and Artery Treatments!
We depend on our blood vessels. They’re a vital part of our cardiovascular system, and without them, our body wouldn’t function like it’s supposed to. So when something goes wrong, it’s imperative that you take the necessary steps to treat your blood vessels as soon as possible.
If you’re looking to schedule an appointment with us, or if you’re wondering if your symptoms may indicate signs of a serious disorder, consider taking a look at our vein and artery consultation tool. Just by answering a few of our questions, you can find out if you’re a candidate for one of our treatment programs. Give it a try now.