An issue that many of our patients are concerned about as they receive vein treatments at our clinic is blood clots. Though not always a risk for every patient, potential clotting in the veins is something that we carefully monitor for. But not all blood clots are immediately easy to identify, even with visible or mild symptoms. Some clots form within deeper veins and tissue, proving an issue that can be incredibly dangerous and difficult to pin down. We call the formation of such a clot a deep vein thrombosis.
When a patient at the Ozark Regional Vein & Artery Center develops deep vein thrombosis, we ensure they receive quality DVT treatments in Rogers.
Unmatched Care from World-Class Vascular Specialists

You know Dr. Haney and the incredible team at the Ozark Regional Vein & Artery Center for their work as premier vein experts in Rogers. With patients from all across Northwestern Arkansas, from Bentonville down to Fayetteville, the Ozark Regional Vein & Artery Center can now provide you with world-class arterial disease care in Rogers.
Dr. Christopher Stout, the newest addition to the Ozark Regional Vein & Artery Center family, is a world-class vascular surgeon with specialties in angioplasty, arterial stenting, and limb recovery. Dr. Stout is a world-renowned expert in diagnosing, treating, and managing diseases and conditions affecting arteries and veins.
As we’ve learned from our years of providing care to our community, many people haven’t had the opportunity to learn about vascular health. We’re committed to providing exceptional patient education to everyone we work with.
That’s why we’re taking the time to discuss an often-overlooked health concern that impacts an estimated nearly 1 million Americans each year. This blog will thoroughly answer the most common questions we receive about deep vein thrombosis and review what you can expect from DVT Treatments in Rogers.
The Basics of Deep Vein Thrombosis
Deep vein thrombosis (DVT) occurs when a thrombus (blood clot) develops in veins deep in your body—typically your legs, thigh, or pelvis. This can happen for various reasons but is most often a result of a vein injury or slowed blood flowing through your veins. The blood clots may wholly or partially block blood flow through your vein unless targeted by DVT treatments.
What is the danger of DVT?
Even though DVT itself is not life-threatening, the blood clots have the potential to break free and travel through your bloodstream. A pulmonary embolism (PE) happens when the traveling blood clots get lodged in your lung’s blood vessels. Since this can be a life-threatening condition, you need a quick diagnosis and treatment.
Individuals who contract DVT but do not receive DVT treatments in Rogers often experience leg pain and swelling. These symptoms happen because of damage to your veins’ valves and inner lining, leading to blood pooling more than it should. This increases the pressure inside your veins and causes pain and swelling.
Notable complications of DVT include:
- Pooling of blood
- Chronic leg swelling
- Increased pressure within your veins
- Increased pigmentation or discoloration of your skin
- Leg ulcers
How common is deep vein thrombosis?
It’s the third most common vascular disease, behind heart attacks and strokes. Acute DVT/PE can occur at any age but are less common in children and adolescents and far more common in those over 60. More than half of DVTs happen due to being in the hospital from a medical illness or following surgery. This is because you’re likely lying in bed instead of moving around like you usually would.
What are the symptoms of deep vein thrombosis?
A DVT usually forms in the veins of your legs or arms. Many patients have trouble identifying DVT symptoms in Rogers as they do not experience noticeable symptoms at all. But often, symptoms that do manifest are mild and don’t raise concern immediately. This is why patients don’t always come in for DVT treatments in Rogers as quickly as they should. It’s not their fault; they just don’t know something is wrong until complications arise.
Possible DVT symptoms you should make sure to look out for include:
- Swelling of your leg or arm (sometimes this happens suddenly).
- Pain or tenderness in your leg or arm (may only occur when standing or walking).
- The area of your leg or arm that’s swollen or hurts may be warmer than usual.
- Skin that’s red or discolored.
- The veins near your skin’s surface may be larger than normal.
- Abdominal or flank pain (when blood clots affect the veins deep inside your abdomen).
- Severe headache (usually of sudden onset) and/or seizures (when blood clots affect the veins of your brain).
Some people don’t know they have a DVT until the clot moves from their leg or arm and travels to their lungs. Symptoms of acute PE include chest pain, shortness of breath, cough with blood, lightheadedness, and fainting.
It’s critical to call your doctor right away or go to the emergency room if you have symptoms of a DVT. Don’t wait to see if your symptoms go away. Get any necessary DVT treatments in Rogers right away to prevent serious complications.
What causes deep vein thrombosis?
These conditions can increase your risk of a deep vein thrombosis:
- Inherited conditions that increase your risk of blood clots
- Family History
- Physical Injury
- Recent Surgery
- Inactive Lifestyle
- Prolonged immobility
- Pregnancy
- Age
- Overweight/Obese
- Tobacco use
- Existing varicose veins
- Taking birth control
- Using a pacemaker
How We Identify Deep Vein Thrombosis
How is DVT diagnosed?
Your healthcare provider will do a physical exam and review your medical history. You’ll also need to have imaging tests.

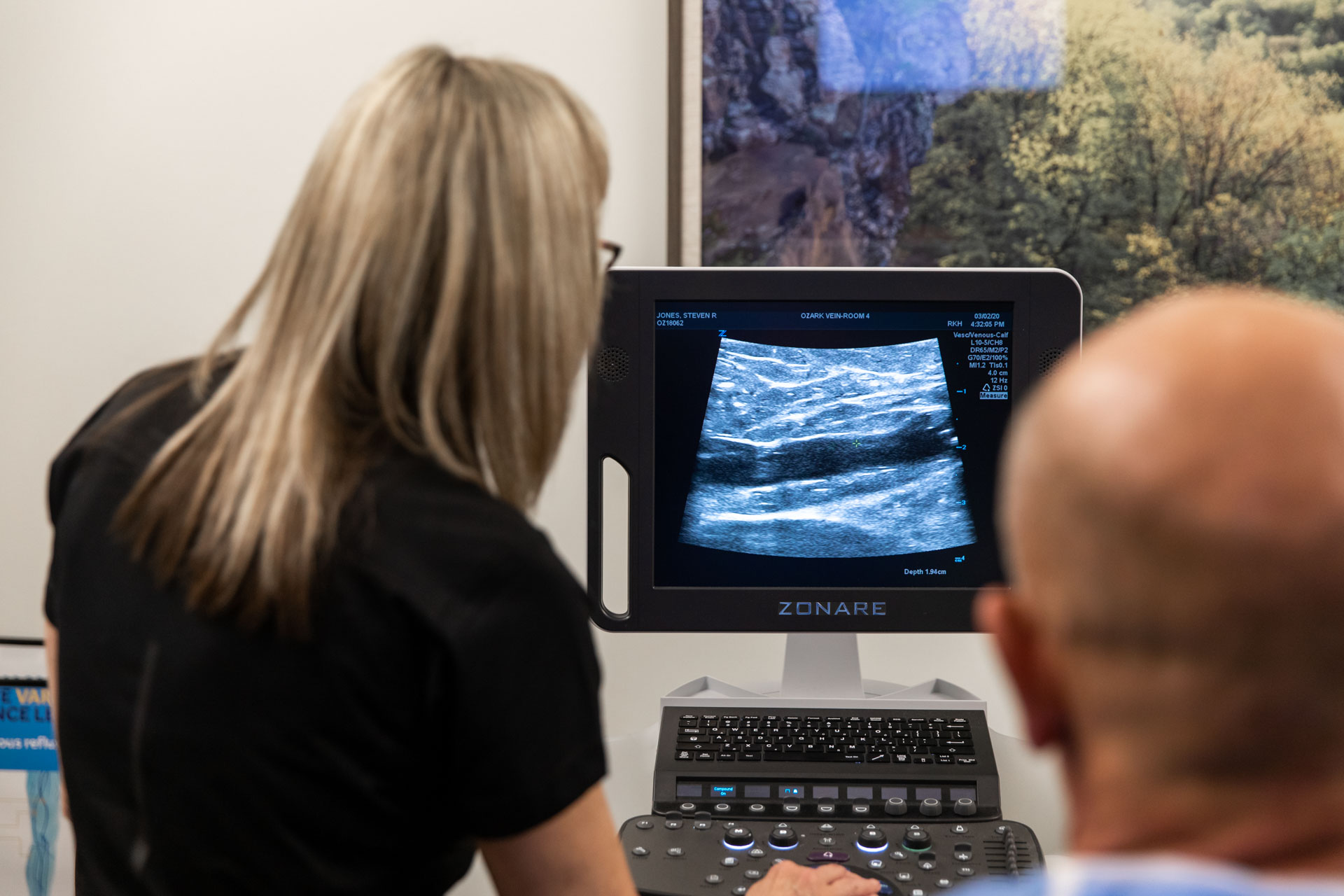
The test we offer at Ozark Regional Vein & Artery Center for DVT Treatment in Rogers is a Duplex Ultrasound. This is the most common test for diagnosing DVT. It uses ultrasound waves to map your blood vessels, allowing us to show blood flow and clots in your veins. During this test, your Ozark Regional Vein & Artery Center provider will apply pressure while scanning your arm or leg. If the pressure they apply doesn’t compress your vein, it could mean a blood clot is present. Unlike hospital appointments, our team can get patients in for testing and provide them with results within 48 hours.
If your doctor thinks you may have a genetic or acquired clotting disorder, you may need special blood tests. This may be important if:
- You have a history of blood clots that your provider can’t link to any other cause
- You have a blood clot in an unusual location, such as in a vein from your intestines, liver, kidney, or brain
- You have a strong family history of blood clots or a clotting disorder
DVT Treatments & Care
A DVT may make it harder for you to get around first because of leg pain and swelling. But you’ll be able to slowly return to your normal activities. If your legs feel swollen or heavy, lie in bed with your heels propped up. This helps improve circulation and decreases swelling.
In addition:
- Exercise your calf muscles
- Stand up and walk for a few minutes every hour while awake
- Wear knee-high compression stockings
- Avoid activities that may cause a serious injury
- Stay hydrated at all times
What treatments are available for people with deep vein thrombosis?
DVT treatments in Rogers include medications called anticoagulants, compression stockings, and elevating your affected leg(s) at different times throughout the day. In a minority of cases, when the DVT is extensive, treatment may require more invasive procedures, like surgery. But broadly, we treat all blood clots in Rogers the same way. The main goals of DVT treatment are to:
- Keep the clot from expanding
- Prevent the clot from breaking off in your vein and moving to your lungs
- Lessen the risk of another blood clot
- Prevent long-term complications from the blood clot
Anticoagulants
Also called blood thinners, anticoagulant medication makes it harder for your blood to clot. Critically, for DVT patients, they also stop clots from getting bigger and from moving. However, blood thinners won’t get rid of blood clots. Your body may naturally dissolve a clot, but sometimes clots don’t completely disappear. When they don’t, they usually shrink and become little “scars” inside your veins.
If you need to take an anticoagulant, you may have to take it for only a few months (usually 3-6 months), or you might take it indefinitely. Your treatment time may be different depending on the specific situations of each individual, including if:
- You’ve had clots before
- You’re getting treatment for another illness, like cancer or an autoimmune disease (you may need to take an anticoagulant if your risk of a clot is higher)
Bleeding is the most common side effect of anticoagulants. You should call your doctor immediately if you notice that you bruise or bleed easily while taking this medication.
Elevate Your Legs
Though this can sound a little ridiculous, elevating your legs while sitting down can naturally help the blood flow toward the heart. This is because your veins won’t have to work against gravity. This can improve circulation and lessen blood reflux in your legs, as well as the strain on your veins caused by a DVT clot. It may be simple, but it’s an incredibly effective behavior for improving your venous health long-term.
Compression Stockings
You‘ll probably need to wear compression stockings to improve or eliminate leg swelling. Damage to the small valves inside your veins often causes this swelling. You may also have swelling because the DVT blocks blood flow in your vein. You wear most compression stockings just below your knee. These stockings are tight at the ankle and become looser as they go away from your ankle. This causes gentle pressure on your leg, which promotes blood flow.
Clinical studies have shown that compression stockings improve the symptoms of leg pain and swelling by at least 50% as long as they’re worn daily during the day.
DVT Treatment Procedures
When you can’t take medications to thin your blood, or you have blood clots while taking blood thinners without missing doses, a surgeon may have to do a procedure to put in an inferior vena cava filter. This IVC filter is placed within the veins to prevent larger dislodged blood clots from reaching your lungs and causing a pulmonary embolism. This treatment option, though effective at preventing PEs, is not a lasting solution. It cannot prevent additional blood clots from forming.
Reducing Your Risk of DVT

After you have a DVT, you’ll need to reduce your risk of future DVT/PE clots by:
- Taking your medications exactly as your healthcare provider tells you to.
- Keeping your follow-up appointments with your doctor and the laboratory. These tell your provider how well your treatment is working.
- Making lifestyle changes, such as eating healthier foods, being more active, and avoiding tobacco products.
If you’ve never had a DVT, but have an increased risk of developing one, be sure to:
- Exercise your calf muscles if you need to sit still for a long time. Stand up and walk at least every half hour if you’re on a long flight. Or get out of the car every hour if you’re on a long road trip.
- Get out of bed and move around as soon as possible after you’re sick or have surgery. The sooner you move around, the less chance you have of developing a DVT.
- Take medications or use prescription compression stockings after surgery. This can help reduce the risk of future blood clots.
Frequently Asked Questions About DVT Treatments in Rogers
What can I expect if I have deep vein thrombosis?
You may need blood tests to ensure you get the appropriate dose of blood thinners. A DVT can take several months to a year to come apart, so you’ll need to keep taking blood thinner medicines as instructed and keep wearing compression stockings until your provider tells you to stop. Your provider may want to do more ultrasounds later to determine if your blood clot is still in the same place, improving, or getting larger.
When should I see my healthcare provider?
You should see your healthcare provider if treatment does not seem to be improving your symptoms. You should also inform your provider if you notice that you bruise easily or have heavy periods during your treatment. These can be signs that your condition is not improving, and more invasive DVT treatment methods may be necessary.
How long will I need to take blood thinners?
You can expect to take blood thinners as part of DVT treatments in Rogers for at least 3-6 months. This timeline may vary depending on which medication you use. Some patients may need to take prescription anticoagulants for a longer time if the clot doesn’t break down completely.
When can I travel again?
We recommend patients wait at least 4 weeks after having DVT or PE before traveling any considerable distance, but talk to your doctor. They may have advice or think that you’re recovering smoothly enough that the risk of another provoked DVT is unlikely. They can also help you take any necessary precautions before you travel.
Turn to the Ozark Regional Vein & Artery Center for Quality Vascular Care and DVT Treatments
If you’re looking to undergo DVT treatments in Rogers, come to the Ozark Regional Vein & Artery Center. Our experience and growing suite of care options allow us to guide you toward lasting wellness solutions for a happier, healthier life.
We are a premier practice in Northwest Arkansas for the highest-quality vein treatments. Dr. Haney, Dr. Stout, and the expert staff have over 500 years of combined experience in the industry. Patients come to Dr. Haney from all over Northernwestern Arkansas, from Fayetteville to Bentonville, to ensure they receive the best concierge-level care and leg vein procedures.
Take the first step on the road to recovery with our Virtual Vein & Artery Screening Quiz, or schedule a consultation!
We also hold regular free screening events. Sign up for our newsletter to be notified of our free public events and other practice specials!